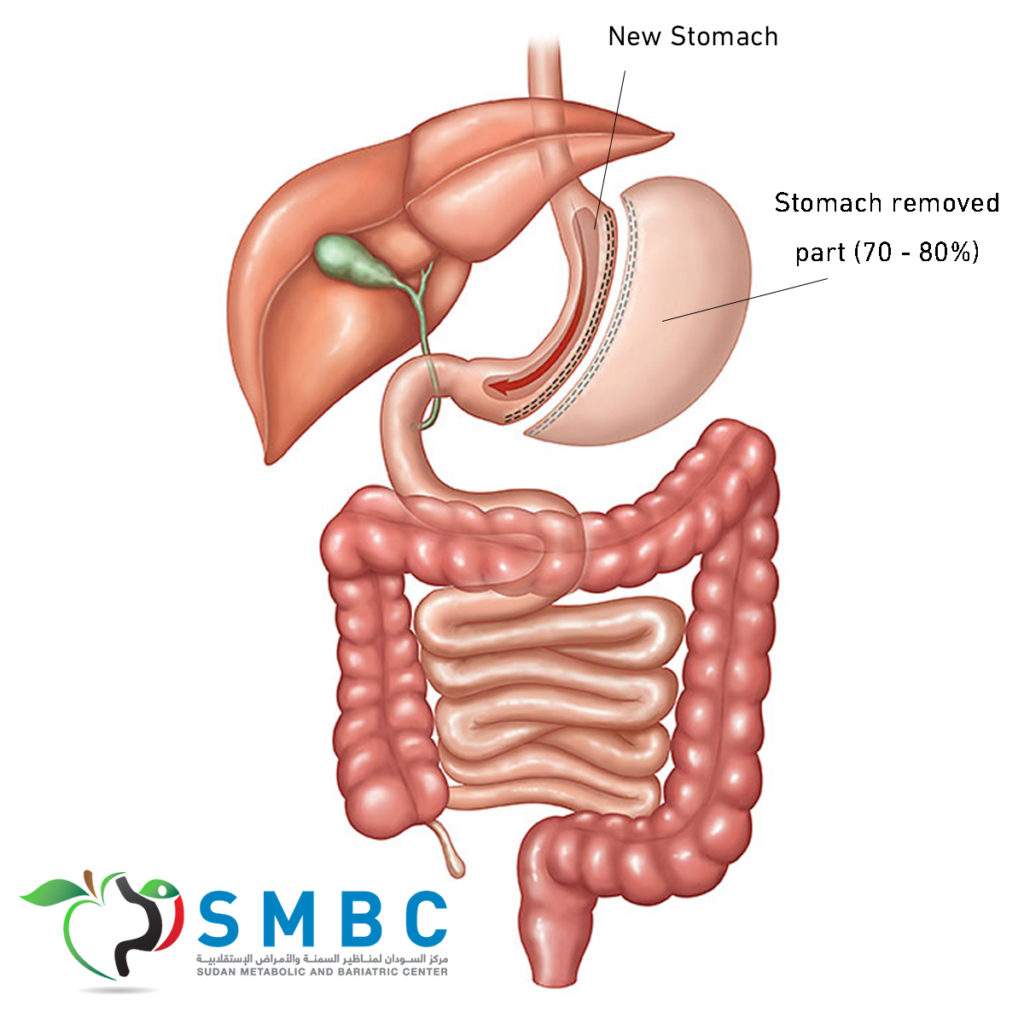
Laparoscopic Sleeve Gastrectomy is an effective bariatric procedure. Estimated weight loss is almost as big as with gastric bypass and simultaneously gastric sleeve is more “natural” as food continues to pass through all the parts of gastrointestinal tract. Sleeve gastrectomy technique has perfected considerably over recent years towards slimmer and longer sleeves with complete removal of gastric fundus yielding better and durable weight loss.
In this operation, 85% of the stomach is removed and a banana-shaped gastric tube with a diameter of approximately 2-2.5 cm and volume of 100-150ml/3.4-5 fl. oz is formed. This reduces the gastric volume and the quantities of food ingested. In comparison, an average sized normal stomach of medium fullness is 1-1.5 litres / 34-50 fl. oz. The surgery is always performed laparoscopically.
The main difference of sleeve gastrectomy compared with bypass surgery is that, in the case of gastric sleeve, food still flows through every part of the digestive system and therefore the absorption of nutrients (including vitamins and minerals) and medications is not affected. After the surgery, the stomach and duodenum can still be examined laparoscopically , which is important for patients with certain types of stomach and biliary diseases.
How does Sleeve Gastrectomy work?
Gastric Sleeve surgery reduces appetite (hunger) and the amount of food eaten. Appetite is reduced because the part of stomach that produces the hunger hormone ghrelin is removed. A stomach reduced in size to 100-150 ml / 3.4-5 fl. oz. as opposed to the normal size of 1500 ml / 50 fl. oz. fills up remarkably more quickly and the feeling of satiety is achieved by swallowing just a couple of mouthfuls. Also the faster flow of food from the stomach’s tube to the small intestine plays a role in the reduction of appetite, as the small intestine’s contact with freshly swallowed food amplifies the feeling of a full stomach.
Who should consider Gastric Sleeve surgery?
- a BMI below 45 kg/m2
- aged over 70;
- small bowel adhesions resulting from previous surgeries, making the patient unsuitable for laparoscopic bypass surgery;
- a preference not to have to use as many vitamins and food supplements as are needed in the case of bypass surgery;
- a propensity to develop anaemia as a result of iron deficiency even prior to the surgery;
- the prospect of getting pregnant and giving birth;
- the need to use a daily dose of pain killers like diclofenac or ibuprofen;
- imminent or freshly performed organ transplant surgery;
- a diagnosed inflammatory bowel disease (ulcerous colitis, Crohn’s disease);
- a potential necessity for future endoscopic access to the stomach and duodenum
Facts about Gastric Sleeve surgery
Long term effects of Gastric Sleeve surgery
There have been many studies conducted on the long term (more than 5 years) effects of gastric sleeve surgery. The loss of weight is expressed as an excess body weight loss percentage. A survey review article analysing 16 original studies concluded that 5 years post-surgery the average excess body weight loss was 62.3% (ranging from 52% to 69% in the different studies examined). 7 years after surgeries the patients had lost on average 67% of their excess body weight. The percentage of weight loss was greater in those with a pre-surgery BMI below 45 kg/m2
Important! In cases where body weight loss is insufficient or body weight starts to rise, it is possible to convert a gastric sleeve into a gastric bypass
Many diseases connected to being overweight like sleep apnoea, type 2 diabetes, joint diseases, high blood pressure or polycystic ovary syndrome (PCOS) improve or disappear as a result of gastric sleeve surgery.
Important! As with all medical procedures, individual results and experiences may vary. Long term effects of any gastric surgery are reliant on a patient making the necessary changes to lifestyle, particularly in relation to diet and exercise.
Possible complications after Gastric Sleeve
In our practice the most likely complication after sleeve gastrectomy has been postoperative bleeding (1% of patients). Usually the bleeding stops itself and isn’t so great that the blood transfusion is needed.
Other early complications (occurrence 0,5%) may be: peritonitis; thrombus of deep veins and lung artery; myocardial infarction; pneumonia; abdominal abscess; wound infections; narrowing of the stomach tube; difficulties in swallowing.
Later side effects after gastric sleeve may be: difficulty in swallowing and pain while eating during the first 1-1.5 months, heartburn (20% of the patients, however, it can be treated with omeprazole), occasional vomiting (rarely longer term), various foods intolerance, dumping syndrome (much more rarely than after bypass) , vitamin B12 and iron deficiency (much less than after bypass), gallstones; constipation; diarrhoea; excess skin; loss of hair.
Pros & Cons of the Gastric Sleeve surgery
• Excess body weight loss of 60-70%.
• Improved quality of life for 95% of patients.
• The food flow in the digestive system doesn’t change.
• Remission of type 2 diabetes: 55-60%.
• Remission of sleep apnoea and snoring: 90%.
• Disappearance or major relief from back and joint pain.
• Reduced risk of developing dumping syndrome compared to bypass surgery.
• Mortality rate of the surgery is low: less than 0.1%.
• The risk of serious surgical complications (ones that need reoperation, blood transfusion or a hospitalisation of more than 1 week) is low: 1,5%.
• Complications as a result of reduced absorption of vitamins and minerals are much more rare compared with bypass surgery.
• The stomach and duodenum remain endoscopically examinable.
• Weight loss is a little lower compared with bypass surgery.
• Increased risk of weight re-gain in the years following surgery.
• Not suitable for patients with a sweet tooth.
• Increase in heartburn frequency in 20% of patients.
• Reversal of the procedure and restoration of the original anatomy is not possible.
• Increased recovery time compared with bypass surgery.
Summary
To summarise, sleeve gastrectomy results in somewhat lower excess body weight loss than a gastric bypass but is technically easier to perform and helps to avoid certain specific adverse effects of bypass surgery like vitamin and mineral malabsorption. This operation is indicated in particular for those whose BMI is under 45kg/m2 or for those for whom a laparoscopic bypass operation would be difficult to perform due to small intestinal adhesions as a result of previous surgeries.